Dupuytren’s Disease
A fibroproliferative disorder of the hand characterized by the development of new tissue in the form of nodules and cords resulting in a progressive contracture of the fingers into the palm.
It is a common genetic condition more prevalent in men with increasing age. Presentation is most frequently in a person in their 50s or 60s but rarely presents in late teens and the youngest person I have needed to operate on was 23. Generally, the younger the presentation the more aggressive the disease process.
Dupuytren's is commonest in those of Scandinavian, northern UK/ European descent and there is a theory it is related to the Vikings spreading their genes!
Although a genetic predisposition is necessary there are other contributing factors including trauma; commonly an injury (wrist or hand fracture or wound) can trigger the process or accelerate existing disease. Patients with a Dupuytren's disposition also seem to get more stiffness (and probably soreness) after an injury. It is important to understand that surgery is a form of trauma, no matter how nicely it is done!
The nodules can be sore in early disease (settles with time) but pain is not a prominent feature and is never an indication for surgery in Dupuytren's disease.
There is no cure for Dupuytren's but many good treatment options. It is always progressive ( worse over time) but in a somewhat unpredictable fashion. Unfortunately, the outcomes from surgery can also be a bit unpredictable!
History
First description credited to Felix Plater (1614, Basel Switzerland).
Dupuytren’s Diathesis
This is a spectrum of physical findings in patients with particularly strong gene expression. Patients may present at a young age and have very aggressive cord development.
These patients also have multiple digit involvement and disease is always bilateral. Other features can include Garrod’s nodes (knuckle pads), Lederhose’s disease involving the feet (plantar fibromatosis) and Peyronie’s disease (penile fascia involvement).
The significance of having a Dupuytren's diathesis (more aggressive disease) include having a higher risk of poor surgical outcomes or early recurrence. Collagenase injections (in early disease) may be helpful to delay surgery and if surgery is necessary, skin grafting is generally indicated to decrease/ delay recurrence.
Pathology of nodules and cords
Clinical Presentation
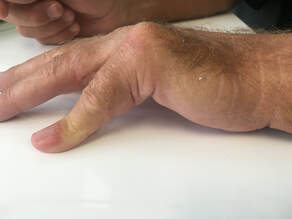
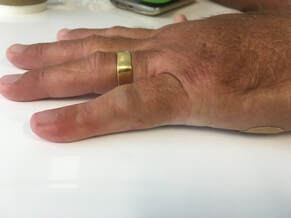
Table top test of Hueston – place hand and finger flat on table
Functional impairment – affected finger gets in the way of:
Treatment
On initial presentation this is usually non-operative. Education and reassurance that this is a benign (but annoying) condition is important
Operative
• In my practice, local anaesthetic procedures such as needle fasciotomy and percutaneous fasciotomy have essentially been replaced by Collagenase injections
• Open surgery (selective fasciectomy)
PIP (proximal finger) joint release
Surgical risks
• long term recurrence is about 50%
• skin/ flap necrosis - usually heals with dressings only
• Nerve/ vessel injury - more likely with severe disease
• Complex Regional Pain Syndrome (CRPS)
Post-operative management/ rehabilitation
• Hand therapy is extremely important in achieving a good result
• night splint (maintaining extension) for 3 - 4 months
• out of plaster/ splints and moving early; using the hand during the day in the first week
• swelling/ oedema control helps decrease the resistance to movement (and pain)
• wound and scar management
Fig 1: failed table top test
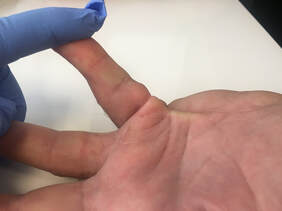
Fig 2. cord with maximum passive extension
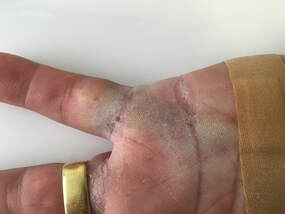
Fig 3 and 4. immediately post Xiaflex and manipulation
It is a common genetic condition more prevalent in men with increasing age. Presentation is most frequently in a person in their 50s or 60s but rarely presents in late teens and the youngest person I have needed to operate on was 23. Generally, the younger the presentation the more aggressive the disease process.
Dupuytren's is commonest in those of Scandinavian, northern UK/ European descent and there is a theory it is related to the Vikings spreading their genes!
Although a genetic predisposition is necessary there are other contributing factors including trauma; commonly an injury (wrist or hand fracture or wound) can trigger the process or accelerate existing disease. Patients with a Dupuytren's disposition also seem to get more stiffness (and probably soreness) after an injury. It is important to understand that surgery is a form of trauma, no matter how nicely it is done!
The nodules can be sore in early disease (settles with time) but pain is not a prominent feature and is never an indication for surgery in Dupuytren's disease.
There is no cure for Dupuytren's but many good treatment options. It is always progressive ( worse over time) but in a somewhat unpredictable fashion. Unfortunately, the outcomes from surgery can also be a bit unpredictable!
History
First description credited to Felix Plater (1614, Basel Switzerland).
- Henry Cline (1808, London)described typical palmar fibrosis and flexion contractures and recommended surgery.
- Astley Cooper (1822) also described finger contractures in A Treatise on Dislocations and Fractures of the Joints
- Guillaume Dupuytren (1777-1835, Paris) published a description of 2 patients with palmar fibromatosis in 1834 and managed to get his name attached to the disease!
- May be autosomal dominant with variable penetrance or sporadic (approximately 10% have a positive family history)
• Mainly Scandinavia and Great Britain
• Rarer in Southern Europe
• Common in Australia due to British/ Irish immigration
• virtually unknown in Greece, Middle East and orient • though Indians living in the UK have developed disease so there may be an environmental component
Dupuytren’s Diathesis
This is a spectrum of physical findings in patients with particularly strong gene expression. Patients may present at a young age and have very aggressive cord development.
These patients also have multiple digit involvement and disease is always bilateral. Other features can include Garrod’s nodes (knuckle pads), Lederhose’s disease involving the feet (plantar fibromatosis) and Peyronie’s disease (penile fascia involvement).
The significance of having a Dupuytren's diathesis (more aggressive disease) include having a higher risk of poor surgical outcomes or early recurrence. Collagenase injections (in early disease) may be helpful to delay surgery and if surgery is necessary, skin grafting is generally indicated to decrease/ delay recurrence.
Pathology of nodules and cords
- Nodules and cords are pathological (abnormal) structures in the (normal )palmar fascia. The palmar fascia (or aponeurosis) is a complex 3 dimensional fibrous structure which acts as a framework for longitudinally running structures (tendons and nerves). It is deep to skin and fat but inserts into skin and extends into the fingers. Nodules are dense cellular collections of myofibroblasts which are the abnormal cell in Duputyren's. The nodules produce flexion contractures by pulling through cords (of abnormal fascia) that have extended past the finger joints.
- There are various abnormal cords that form, but particularly of note in the fingers, the spiral cord contracts and displaces the neurovascular bundles towards the midline and superficially making them prone to injury during surgery or even injections.
Clinical Presentation
- Men to women >7:1
- Less severe or atypical in women
- The nodule forms first but may disappear as disease progresses
- or may present when tender nodule or noticed
- can present late with severe joint restriction if the disease is completely painless (common)
- often referred (incorrectly) as a trigger finger or “joint stiffness”
- The progression is unpredictable
Table top test of Hueston – place hand and finger flat on table
- If your hand can go flat then surgery is usually not indicated
- this correlates with MCP (knuckle) joint contracture>30 deg
Functional impairment – affected finger gets in the way of:
- Washing your face/combing hair
- Putting your hand in your pocket
- Racquet sports or golf
Treatment
On initial presentation this is usually non-operative. Education and reassurance that this is a benign (but annoying) condition is important
- Disease is often mild and may never require surgical treatment
- Progression of the disease is very difficult to predict
- Stretching, massage or exercises do no harm but make no difference to outcome
- A steroid injection may relieve soreness in a very tender nodule (not useful in cord disease) or for knuckle
pads
Operative
• In my practice, local anaesthetic procedures such as needle fasciotomy and percutaneous fasciotomy have essentially been replaced by Collagenase injections
• Open surgery (selective fasciectomy)
- aim is to excise the diseased fascia to release contractures
• preserving main nerves and vessels - maintaining full flexion of the fingers (avoiding stiffness)
- combination of longitudinal and zig-zag (Brunner) incisions used with techniques to lengthen skin wounds (move skin from the side to gain length)
- may decrease recurrence by bringing in normal skin
- BUT potentially slows rehabilitation resulting in more stiffness AND altered sensation, poorer wear characteristics (to normal skin) and poorer cosmesis
- important to use in severe disease/ Dupuytren’s diathesis or in revision (2nd) surgery
PIP (proximal finger) joint release
- controversial
- if the joint is still bent after cord excision the joint is often released
- BUT may result in significant stiffness
- AND difficult to maintain initial results
- therefore I only perform joint releases if a severe contracture persists after cord excision; it is more important to be able to bend the finger easily after surgery than have a perfectly straight finger
Surgical risks
• long term recurrence is about 50%
• skin/ flap necrosis - usually heals with dressings only
• Nerve/ vessel injury - more likely with severe disease
• Complex Regional Pain Syndrome (CRPS)
- difficult to predict and approximately 5% will develop
- results in stiffness and often a poor result
Post-operative management/ rehabilitation
• Hand therapy is extremely important in achieving a good result
• night splint (maintaining extension) for 3 - 4 months
• out of plaster/ splints and moving early; using the hand during the day in the first week
• swelling/ oedema control helps decrease the resistance to movement (and pain)
• wound and scar management
Fig 1: failed table top test
Fig 2. cord with maximum passive extension
Fig 3 and 4. immediately post Xiaflex and manipulation